
What is Pudendal Neuralgia?
Neuralgia is just a fancy medical word for pain along the nerve distribution or path. Pudendal Neuralgia has to do with the Pudendal Nerve, the nerve that supplies the genital area in men and women. The Pudendal Nerve supplies sensory fibers to the penis, scrotum, vagina, labia, clitoris and rectal areas. It also provides motor fibers, which means it is responsible for the function of the pelvic floor muscle. These muscles are responsible for normal urinary, bowel, and sexual function as well as a key component of spine, hip and pelvic stability. If your pudendal nerve is having issues, you may struggle with bowel or bladder problems, you may have nerve pain in the vagina, nerve pain in the vulva, or you may suffer from painful orgasm or inability to orgasm.
Nerves are vulnerable to injury:
- where it travels through tunnels or canals
- where they branch off, especially if they make sharp turns
- where they lie along hard surfaces like bone
- there the system is fixed leaving less room for movement of the nerve
Where is the Pudendal Nerve?
The Pudendal Nerve arises from the sacrum, the bone at the base of the spine. It travels through a fascial sleeve, the Alcock’s Canal, makes a sharp turn along the ischial tuberosity (a bone) and has several branches that make sharp turns to supply the penis or clitoris, rectum and perineum. This is a perfect storm for nerve injury or irritation.
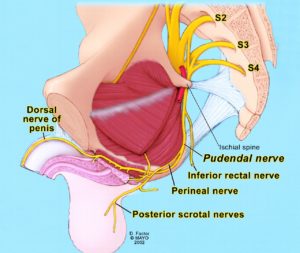
Causes of Pudendal Neuralgia:
Nerves love movement and blood flow. When they are compressed by lack of space, direct pressure on the nerve, or muscle tension, this causes decreased blood flow and poor ability to slide through the tissues. This causes pain or poor firing of the nerve. The result is poor muscle function to the muscles the nerve supplies. In this case – the pelvic floor muscles. Nerves also can be injured by traction or constant stretching. This can happen with repetitive motions or prolonged positions. Chronic infections can also irritate a nerve due to the inflammation surrounding it. These both cause pain or muscle dysfunction. It is very important to consider the tissues surrounding the nerve as well as the patient’s daily routine, activities and history.
In the case of the Pudendal Nerve, compression can result from chronically tight pelvic floor muscles which can be caused by many factors: muscle guarding after surgery, scar tissue, over-activity due to weakness elsewhere or high level of exercise. Compression can also come from constant sitting at work, with poor postures with sitting jobs, or with recreational activities such as cycling.
Traction injuries to the pudendal nerve can result from childbirth, with prolonged pushing during delivery or extreme hip flexion posture for prolonged periods. It can also be caused by chronic straining with constipation or with heavy lifting. It can also be injured with repetitive deep squatting with weight lifting or work postures. Inflammation from chronic infections like yeast infections or bacterial vaginitis can also be aggravating factors for pudendal nerve.
Diagnosing Pudendal Nerve Pain
Pudendal nerve pain is often misunderstood as the genital area is somewhat of a “no man’s land” when it comes to muscle and nerve. Doctors can easily screen pelvic organs and will find nothing to report, so no explanation of the pain. This causes increased stress in the patient and often increases pain, as stress is a very strong mediator of nerve pain. It is important to consider how stress may play a part in nerve pain and incorporate stress management techniques as part of the treatment plan.
What Does Pudendal Nerve Pain Feel Like?
Nerve pain can take on many descriptors. It can be felt as burning, itching, buzzing or sharp pain. The Pudendal nerve causes pain at the rectum or anus, the sit bones, the perineum (the area of skin between the anus and penis or vagina) the labia, clitoris or penis and scrotum in men. It is often worse with sitting, bowel movements or urination. Sometimes there is pain with sexual intercourse, or other activities such as cycling, running or exercise. Some patients find relief with exercise. Every person with pudendal neuralgia has a different presentation. This is why it is important to see a health care provider who can look head to toe to determine any structural or tissue findings that may be contributing to the pain.
Physical Therapy for Pudendal Neuralgia
Physical Therapy for pudendal neuralgia will examine skeletal structure, movement patterns and muscle recruitment patterns, muscle overactivity or weakness and functional tasks to determine what may be causing the nerve injury. Physical therapists are also trained to manage chronic pain, finding pain relief through stress management, education and movement strategies as well as teaching meditation and mindfulness exercises to help calm the nervous system. If you suffer from any symptom of pudendal neuralgia, you should find a physical therapist who is trained in pelvic floor muscle dysfunction to get help.
Sarah Dominguez PT, MSPT, CLT, WCS
Disclaimer: This blog is here for your help. It is the opinion of a Licensed Physical Therapist. If you experience the symptoms addressed you should seek the help of a medical professional who can diagnose and develop a treatment plan that is individualized for you.









