
Pelvic Pain: Male Symptom Checker
Just because the CT scan, sexually transmitted infections, urinary tract infections, urine and blood tests are negative, doesn’t mean that we, as healthcare providers, can wash our hands of determining the cause of someone’s pain. As physical therapists, our expertise lies in the evaluation and treatment of musculoskeletal conditions. Therefore, if an individual is having pain, and medical tests do not show any abnormalities, the culprit may be a muscular or joint dysfunction, and it is our job to determine this. At Foundational Concepts we specialize in treating pelvic pain in men. Many people don’t realize that men can experience pelvic floor dysfunction, and it is this misconception that contributes to the delayed diagnosis and treatment of these patients.
As women, we’re used to dealing with occasional discomfort in our private areas. Most of us have experienced a urinary tract infection, a yeast infection or even a painful period at some point in our life. Others have even had to face chronic pelvic pain or pain with intercourse (dyspareunia). Fortunately, many women see a healthcare provider on an annual basis and have the resources to address these conditions. However, most men do not go to the doctor as much, and therefore are not aware of the services that exist for pelvic pain in men.
Here is a symptom checker for men with pelvic pain:
Often, when a man has pelvic pain he will report pain between his testicles and his anus. He may experience abdominal pain. This sensation may intensify with sitting, exercise, intercourse, urination or a bowel movement. The individual may notice that he is urinating more frequently, having increased “urgency” or even an inability to fully empty his bladder. He may experience a slow or hesitant urine stream. He may notice pain with erection or orgasm. A physician will usually evaluate this type of condition with a rectal exam. If this exam is painful, the physician may conclude that there is inflammation of the prostate. However, many times, the prostate is not actually inflamed, and it is actually pelvic floor muscte tension.
– Stress- Chronic strain from biking, sitting, heavy lifting, coughing etc.
– A pelvic malalignment, such as sacroiliac joint dysfunction
– Lower back pain
– Hip pain
– Surgery in abdomen, groin, hip or back
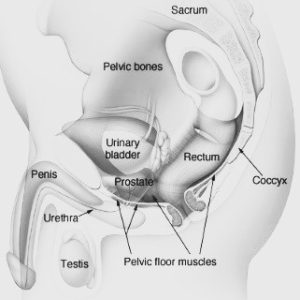
Let’s Talk About the Male Anatomy: Yes, men have a pelvic floor, too!
As shown below, the pelvic floor muscles are suspended from the pubic bones to the tailbone, and they have 4 major functions:
– Sexual excitation
– Sphincter control of urine/stool
– Support of pelvic organs (bladder, bowels, prostate)
– Stabilization of the Lumbo-pelvic region
Disclaimer: This blog is here for your help. It is the opinion of a Licensed Physical Therapist. If you experience the symptoms addressed you should seek the help of a medical professional who can diagnose and develop a treatment plan that is individualized for you.










Comments (0)