Joint Hypermobility: Too much flexibility could be a missed clinical diagnosis.
Hypermobility Spectrum Disorder
People with hypermobility spectrum disorder (HDS) tend to have joint hypermobility and instability making them more prone to injury and pain. However, these patients do not have other connective tissue disorders. Hypermobility describes a joint that is able to move past the normal range of motion. When a joint moves beyond its normal range, the muscles, tendons, bones, and ligaments are also pulled beyond there normal range which can lead to pain and injuries to the joint and surrounding soft tissues. This can cause acute pain and limit the ability to use the joint. However, sometimes pain and injury doesn’t occur with one big event like a dislocation. Because of the instability of the joints, little tears or traumas can occur to the surrounding areas that may not hurt when the occur, but over time the little traumas can develop into recurrent injuries or a cycle of persistent pain.
Opening the door to persistent pain
Pain is a normal response to inflammation and trauma. When the injury continues to occur, such as continuous subluxation of a joint or an instability in a joint, the nerve surrounding the tissues continue to be irritated and the brain becomes hyperaware of that area of the body. This creates even more sensitivity to pain. We call this hyperalgesia (increased sensitivity to feeling pain and an extreme response to pain). We have talked a lot about pain in some of our other blogs. People with hypermobility may also have decreased proprioception: awareness of where they are in space and how their body needs to work to complete the task at hand.
How do I know if I am hypermobile?
Knowing if you have hypermobility is a good place to start on the path to protecting your body. The Brighton Scoring System is the gold standard tool. This scale is a quick way to assess for hypermobility. There are 5 steps to taking the assessment. A score of 0-3 is considered within normal range while a score from 4-9 is considered hypermobile.
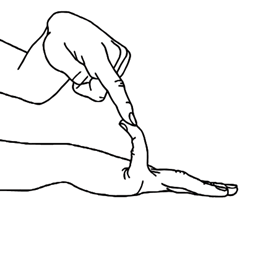
- Pinky fingers. Test both sides: Rest palm of the hand and forearm a flat surface with palm side down and fingers out straight. Can the fifth finger be bent/lifted upwards at the knuckle to go back beyond 90 degrees? If yes, add one point for each hand.
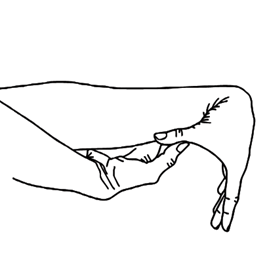
- Thumbs. Test both sides: With the arm out straight, the palm facing down, and the wrist then fully bent downward, can the thumb be pushed back to touch the forearm? If yes, add one point for each thumb.
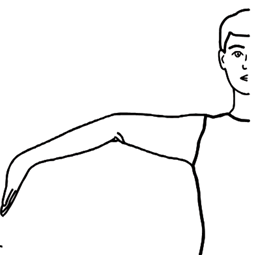
- Elbows. Test both sides: With arms outstretched and palms facing upwards, does the elbow extend (bend too far) upwards more than an extra 10 degrees beyond a normal outstretched position? If yes, add one point for each side.
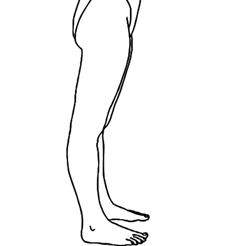
- Knees. Test both sides: While standing, with knees locked (bent backwards as far as possible), does the lower part of either leg extend more than 10 degrees forward? If yes, add one point for each side.
- Spine. Can you bend forward and place the palms of your hands flat on the floor in front of your feet without bending your knees? If yes, add one point.
Finding a Diagnosis
While EDS and HSD are not curable, they are treatable. Having a diagnosis can help in knowing where medical issues are coming from and why they continue to happen. All the subtypes except hypermobile EDS are able to have a genetic test for confirmation of the diagnosis. A clinical geneticist can do the necessary lab work, and many are doing visits via telehealth, decreasing the expense to see providers. As EDS and HSD are not fully understood by the medical community, it is also important to find reputable information and be able to educate yourself on EDS and HSD. A good place to start is the EDS Foundation. Home – The Ehlers Danlos Society : The Ehlers Danlos Society (ehlers-danlos.com)
It is important to develop a network of providers that understand EDS or HSD and their cluster of symptoms. This should include a physical therapist who understands hypermobility and joint protection strategies. Because of the increased elasticity of the skin and decreased stability of joints, it is important to not overtax the system and to focus on stability of the joints and surrounding soft tissue to limit the risk of injury. A pelvic floor physical therapist is an important part of the team. Due to the increased mobiltiy of the connective tissue of the pelvic organs and muscles, people with EDS and HSD have a higher risk of pelvic organ prolapse, constipation, bladder issues (leaking or retention), and pain. Pelvic floor therapists who have a working knowledge of hypermobility will be a huge advocate and educator in management or prevention of symptoms.
Contact us!
A physical therapist with experience with EDS and pelvic health can help you find a doctor, mental health provider and any alternative therapy providers that may be helpful to you. We offer a free 15 minute phone consultation to answer questions and make sure our practice is the right fit for you. Click here to schedule your free consultation!
Disclaimer: This blog is here for your help. It is the opinion of a Licensed Physical Therapist. If you experience the symptoms addressed you should seek the help of a medical professional who can diagnose and develop a treatment plan that is individualized for you.